Healing Between Certainty and Ambiguity — A Child’s Journey Through Immune-Mediated Skin Disease 在确诊与未知之间的疗愈: 一位儿童免疫性皮肤病的康复之路
When a ten-year-old boy first presented to our clinic with persistent reddish macules across his neck, upper trunk, and both arms, the case appeared deceptively straightforward. On physical examination, Initially presented with asymptomatic, discrete, dull pink to erythematous macules and thin papules, ranging from 0.5 to 2 cm in diameter, without significant scale, itchiness or atrophy. His medical history included allergic rhinitis and pityriasis alba—relatively benign dermatological conditions not usually warranting alarm. However, over twelve months, the lesions progressed to involve approximately 15% of the body surface area (BSA), coalescing into larger patches on the upper back, neck, and proximal arms, defying expectations and resisting standard treatments.
His initial prescription of tacrolimus (Protopic) cream failed to arrest the spread of the lesions. Instead, the rashes crept up to involve the neck and upper extremities. Despite subsequent trials of topical corticosteroids—some of increasing potency—the lesions neither resolved nor stabilized. Heat and perspiration seemed to trigger erythematous flares, adding an element of environmental reactivity. With the conventional therapeutic route exhausted and lesions spreading, a skin biopsy was performed to rule out sinister possibilities.

Deciphering a Complex Diagnostic Puzzle
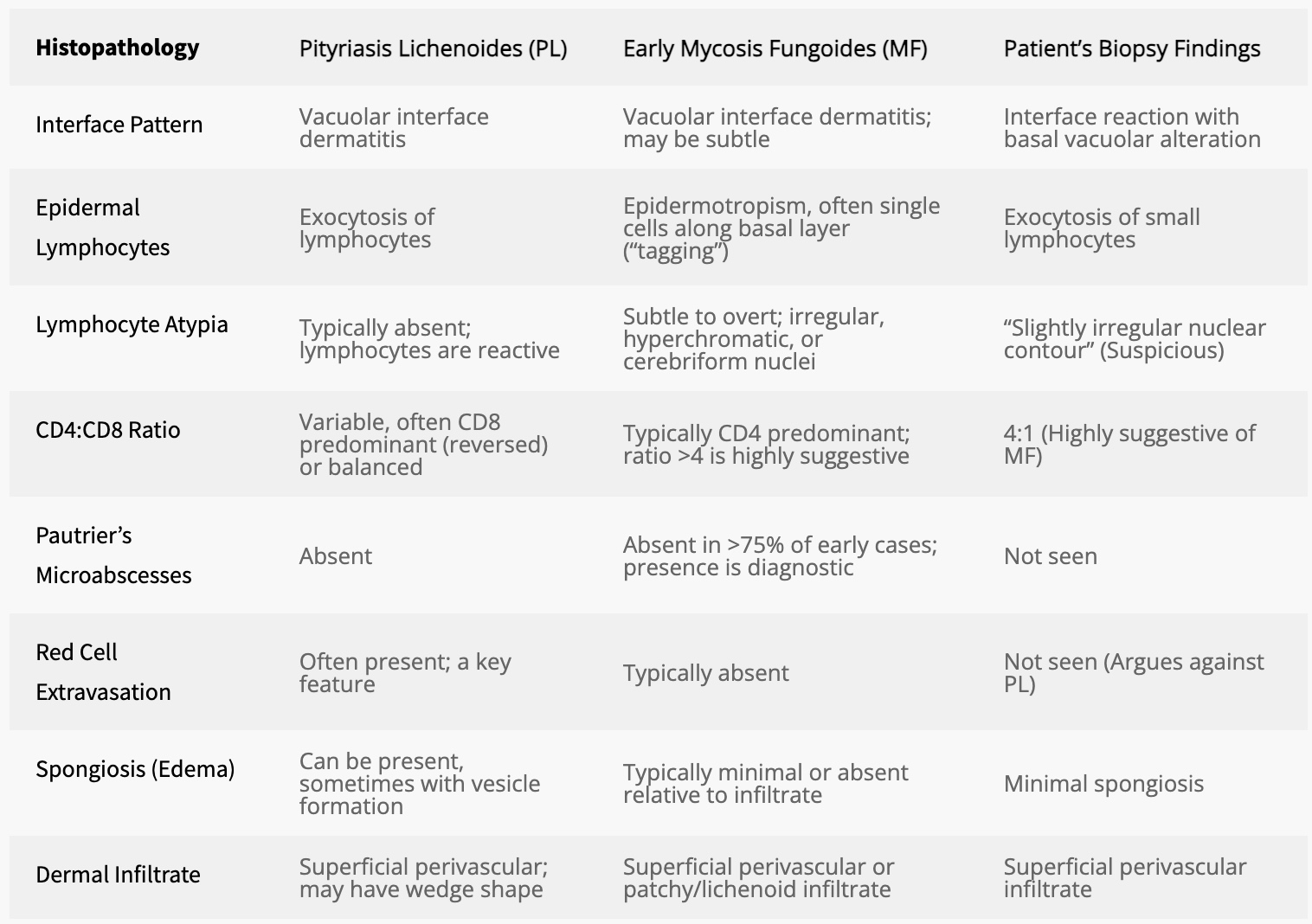
The histopathological report introduced more questions than answers. The primary finding—interface dermatitis—was a descriptive term signaling inflammation at the dermoepidermal junction, but not diagnostic of a specific disease. More concerning was the immunohistochemical finding: a CD4:CD8 ratio of 4:1. This skew toward CD4+ T-helper cells hinted at an early cutaneous T-cell lymphoma—specifically, mycosis fungoides (MF). Yet, key hallmarks of MF such as Pautrier’s microabscesses and marked epidermotropism were absent. Pityriasis lichenoides (PL), a lymphocytic dermatosis, remained a plausible differential. The child had become a diagnostic cipher—a living specimen caught in the gray zone between inflammation and neoplasia.
Treatment
Faced with ambiguity and frustrated by the limitations of conventional management, the parents sought an alternative approach. They arrived at TANGS Clinical TCM, requesting a treatment that aligned with their child’s physiological delicacy and their reluctance to pursue further biopsies or immunosuppressants. Based on the principle of “clearing heat and draining dampness, banlaning yin & yang,” a dual-pronged plan was initiated: the child was prescribed a customised compound herbal formula to be taken orally twice daily, alongside topical application of a Lite Balm, designed to clear internal heat, drain dampness, and rebalance immune function according to TCM principles.
Faced with this diagnostic uncertainty, the parents opted against further invasive procedures or systemic immunosuppressants and sought care at our clinic TANGS Clinical TCM. The patient’s presentation—red macules aggravated by heat, a rapid pulse, and a red tongue with a greasy coat—led to a TCM pattern diagnosis of Damp-Heat and Blood Heat Stagnating in the Skin. A dual-pronged plan was initiated: the child was prescribed a customised compound herbal formula to be taken orally twice daily, alongside topical application of a Lite Balm, designed to clear internal heat, drain dampness, and rebalance yin & yang immune function according to TCM principles.
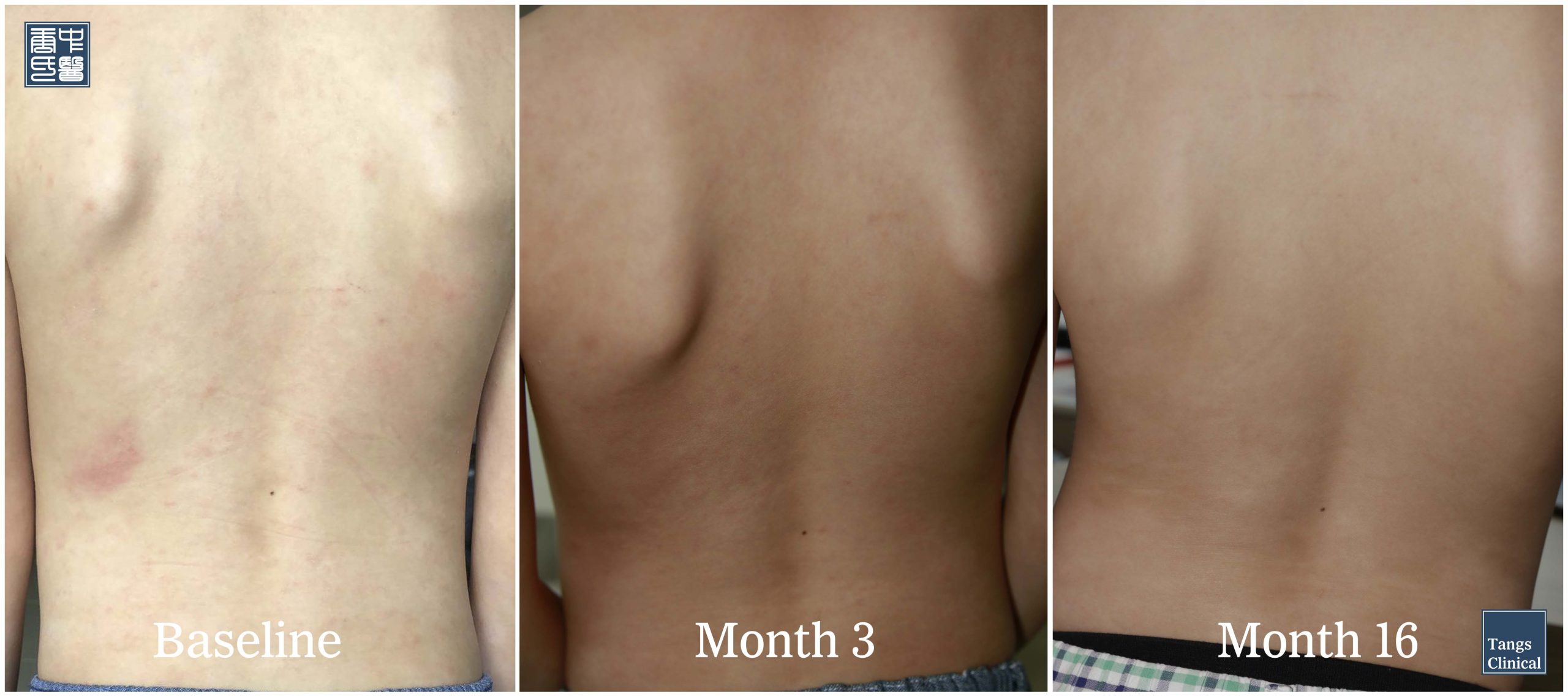
Importantly, the treatment regimen emphasized lifestyle moderation: the child was advised to avoid hot baths, psychological stress, and any further topical or systemic immunosuppressants. Monthly photographic records were taken to track visible progress, and annual blood chemistry profiles monitored internal safety. This careful balancing of holistic intervention and biomedical oversight allowed a rare window into how alternative medicine might manage immune-mediated dermatoses without compromising patient safety.
At the three-month follow-up, a 30% reduction in BSA was noted, with significant fading of erythema in the oldest lesions. By six months, more than 70% of the lesions had resolved into faint post-inflammatory hyperpigmentation. Complete clinical resolution, with restoration of normal skin tone and texture, was achieved at 16 months, and the patient has remained disease-free for the subsequent 5 years of follow-up. The parents, once plagued by fear of a lymphoma diagnosis, now witnessed their child’s skin restored without chemotherapy, without long-term steroids, and without scarring—only herbs, patience, and time.
Discussion
In retrospect, this case underscores not only the difficulty of diagnosing early-stage immune-related skin diseases, but also the value of flexible, integrative thinking. The skin biopsy may have whispered the possibility of MF—but lacking definitive architecture, it could not command a final judgment. Conventional treatments, grounded in immune suppression, had failed to deescalate the dermatosis. In contrast, the herbal regimen, rooted in pattern-based diagnosis and systemic rebalancing, appeared to succeed in promoting immune homeostasis—if not by eradicating a malignancy, then by restoring cutaneous equilibrium.
The outcome should not be misinterpreted as a call to abandon evidence-based medicine. Rather, it invites a more capacious epistemology—one in which ambiguity is not an impasse but a provocation for pluralistic thinking. In the quiet recovery of this child, we find a compelling, if anecdotal, reminder: not all immune dysregulation requires suppression; some may yield to restoration.
While anecdotal, this case raises crucial considerations:
- Immunomodulation Beyond Suppression
Conventional dermatological treatments often rely on immune suppression (e.g., corticosteroids, calcineurin inhibitors), which may risk rebound flares, as seen here. In contrast, TCM may operate through gentler immune recalibration rather than blunt suppression—an approach potentially more suitable for chronic, indolent immune dysregulation - A Systems-Based Framework for Complex Skin Disease
TCM inherently treats the body as a complex, dynamic system. Its pattern-based diagnosis may offer advantages in treating early-stage or borderline cases not yet fitting clear biomedical categories. This framework may be especially helpful in pediatric or subclinical MF, where conventional algorithms offer limited clarity. - Noninvasive Therapeutic Monitoring
The combination of visual documentation and conservative blood monitoring enabled longitudinal tracking without subjecting the child to repeated biopsies. This introduces a humane model for managing uncertain cutaneous diagnoses while awaiting either resolution or progression.
Privacy
In situations where the disease information had already been made publicly available (as evidenced by prior articles), genuine names of individuals have been utilized. Conversely, in instances where there was no pre-existing public disclosure or at the explicit request of patients for privacy, pseudonyms have been employed. Furthermore, identities have been deliberately obscured, and certain contextual details and diagnoses have been modified to hinder any attempts at identification. It is essential to emphasize that the patients and encounters described in this work are authentic, and their consent for publication was duly obtained. As responsible authors, we earnestly implore all our readers to honor the privacy and confidentiality of these individuals. Additionally, certain scenarios, assessments, and clinical interventions have been altered to safeguard the anonymity of both patients and healthcare providers.