Individualized Traditional Chinese Medicine in the Management of Steroid-Dependent Chronic Palmar Eczema: A Case Report
Case Presentation
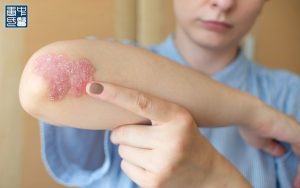
A 25-year-old man with a 15-year history of eczema sought a second opinion due to recurrent disease flares following the cessation of topical corticosteroid therapy. He reported increasing dependence on steroids, with rapid relapse upon withdrawal, prompting him to explore alternative treatment options, including natural therapies and Traditional Chinese Medicine (TCM). He subsequently commenced individualized TCM treatment at our clinic.
The patient was otherwise healthy, with no personal history of atopy and no family history of atopic disease. He had experienced mild eczema since the age of 10, which had remained largely untreated and stable for many years. Two years prior to presentation, he developed a severe flare without identifiable triggers. He was prescribed clocortolone pivalate solution (Cloderm), which resulted in significant improvement of pruritus and skin lesions. However, symptoms recurred upon completion of the 50 mL course, with disease progression from the scalp to the palms.
Subsequently, he was treated with betamethasone valerate 0.1% cream (Uniflex) for palmar involvement, while clocortolone pivalate solution was continued for scalp lesions. Despite ongoing topical corticosteroid use, the palmar eczema remained refractory, characterized by persistent fissuring and pruritus.
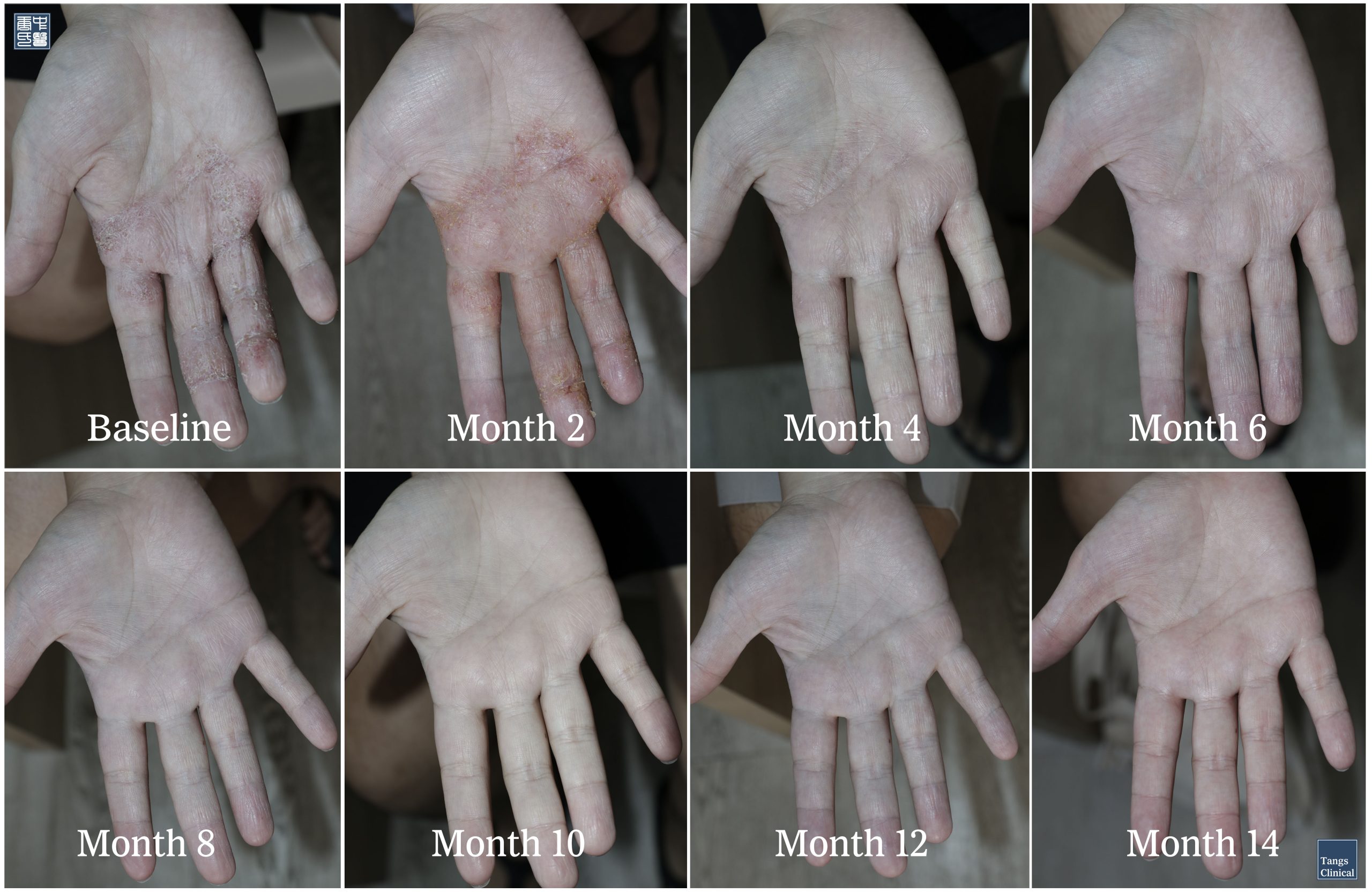
Following initiation of personalized TCM therapy, serial photographic documentation of the patient’s palmar eczema from baseline through Month 14 illustrates a characteristic recovery trajectory following topical corticosteroid withdrawal. During the initial three months, the condition transiently worsened, with increased erythema, scaling, and fissuring, consistent with steroid withdrawal–related rebound inflammation.
From Month 4 onward, progressive epidermal regeneration became evident, marked by the formation of healthier skin layers, reduced inflammation, and gradual resolution of fissures and scaling. Clinical improvement continued steadily on a month-by-month basis. Complete clearance of palmar lesions was achieved by Month 12. Follow-up to Month 14 demonstrated sustained remission, with no evidence of recurrence at the time of reporting.
Privacy
In situations where the disease information had already been made publicly available (as evidenced by prior articles), genuine names of individuals have been utilized. Conversely, in instances where there was no pre-existing public disclosure or at the explicit request of patients for privacy, pseudonyms have been employed. Furthermore, identities have been deliberately obscured, and certain contextual details and diagnoses have been modified to hinder any attempts at identification. It is essential to emphasize that the patients and encounters described in this work are authentic, and their consent for publication was duly obtained. As responsible authors, we earnestly implore all our readers to honor the privacy and confidentiality of these individuals. Additionally, certain scenarios, assessments, and clinical interventions have been altered to safeguard the anonymity of both patients and healthcare